Preimplantation Genetic Diagnosis (PGD) is a cutting-edge technique used during IVF to screen embryos for specific genetic conditions before pregnancy begins. Think of it as a genetic preview, giving you insights into the health of your embryos. This allows us to select embryos that are free from inherited conditions, helping reduce the risk of passing them on to your child.
PGD-A, often referred to as Preimplantation Genetic Screening (PGS), goes a step further. It checks the overall health of the embryo's chromosomes. Chromosomes are like the instruction manuals of our bodies. Sometimes, errors occur, such as missing or extra chromosomes, which can cause implantation failure, miscarriage, or genetic conditions like Down syndrome.
Here’s how PGD-A and PGD-M can improve your IVF journey:
Genetic testing may be a great option if you fall into one or more of these categories:
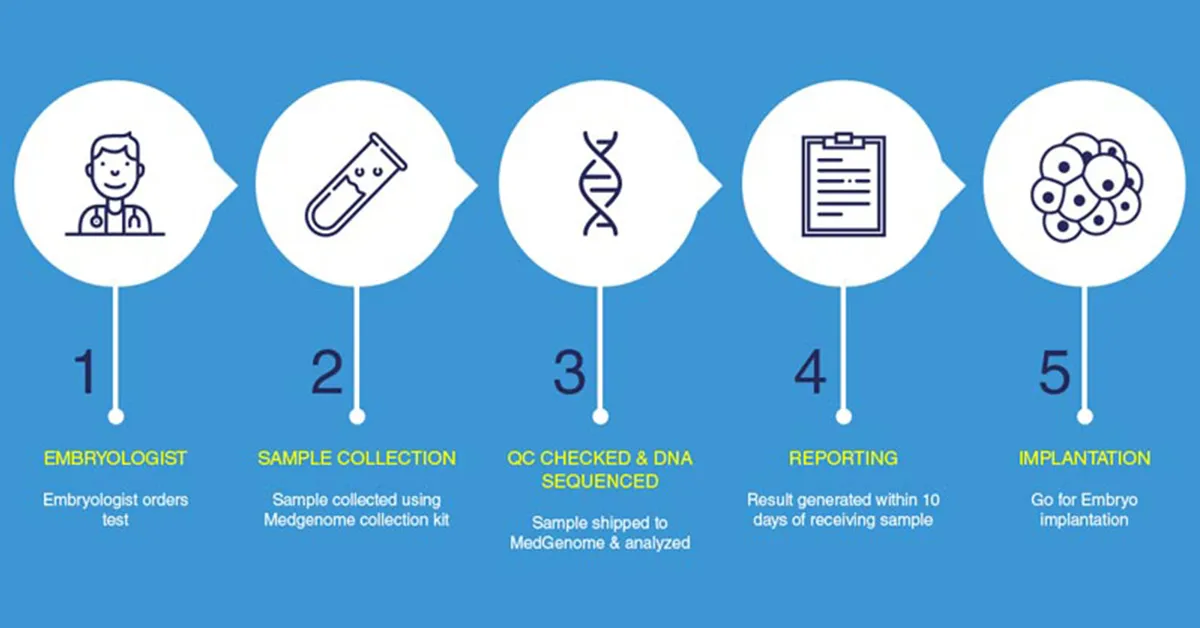
Here’s an overview of how PGD testing works:
The benefits of PGD testing during IVF include:
While PGD testing offers many advantages, there are some factors to consider:
Genetic testing isn’t necessary for everyone, but it can be a valuable tool in certain circumstances. It helps provide peace of mind and confidence in the selection of embryos, especially if you're at higher risk for genetic disorders or have experienced difficulties in your fertility journey. Your fertility doctor can help you assess whether PGD-A or PGD-M is the right choice based on your individual needs.
PGD looks for specific genetic conditions that run in your family, like cystic fibrosis. PGS (now called PGT-A) checks if embryos have the right number of chromosomes. Think of PGD as looking for a specific gene issue, while PGS gives us a general chromosomal health check.
Most embryos handle testing well. We take just a few cells from the outer part of the embryo (the part that becomes the placenta). The inner cells that become the baby stay untouched. But like any procedure, there's a tiny risk.
You'll get results in about 1-2 weeks. During this time, your tested embryos stay safely frozen. Once we know which embryos are healthy, we can plan your transfer. It's better to wait and be sure than to transfer embryos that might not work.
Common reasons for testing are: being over 35, having several miscarriages, failed IVF cycles, or family history of genetic conditions. But it's a personal choice - we'll help you decide if it's right for you.
Using tested embryos can increase your chance of pregnancy per transfer and lower miscarriage risk. But remember - even chromosomally normal embryos don't guarantee pregnancy. It just helps us pick the embryos with the best chance.